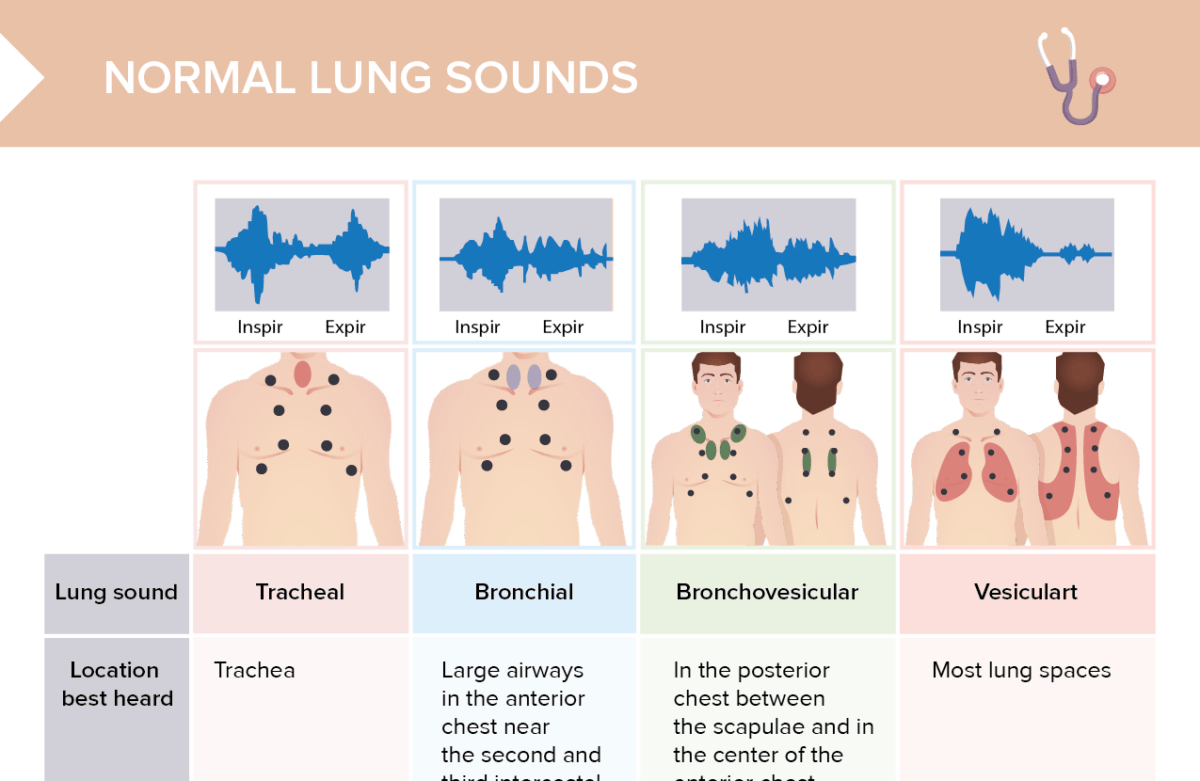
In central PE, chest pain may be from underlying right ventricular (RV) ischemia and needs to be differentiated from an acute coronary syndrome or aortic dissection. Chest pain is a frequent symptom and is usually caused by pleural irritation due to distal emboli causing pulmonary infarction. In patients with preexisting heart failure or pulmonary disease, worsening dyspnea may be the only symptom. Dyspnea may be acute and severe in central PE, whereas it is often mild and transient in small peripheral PE. The most common symptoms of PE include the following: dyspnea, pleuritic chest pain, cough, hemoptysis, presyncope, or syncope. Unfortunately, the diagnosis of PE can be difficult due to the wide variety of nonspecific clinical signs and symptoms in patients with acute PE. It is important to note that 30% of untreated patients with pulmonary embolism die, while only 8% die after timely therapy. Right ventricle (RV) failure due to acute pressure overload is the primary cause of death in severe PE. Given the above pathophysiological considerations, clinical symptoms, and signs of overt RV failure and hemodynamic instability, are indicative of a high risk of early (in-hospital or 30 day) mortality.Ī timely diagnosis of a pulmonary embolism (PE) is crucial because of the high associated mortality and morbidity, which may be prevented with early treatment. As a result, LV filling is reduced in early diastole, and this leads to a reduction in the cardiac output (CO), and cause systemic hypotension and hemodynamic instability. The decreased RV outflow and concomitant RV dilation reduce left ventricular filling, thereby compromising cardiac output. The desynchronization of the ventricles may be increased by the development of the right bundle branch block. Increased PVR increases the right ventricular afterload, which impedes right ventricular outflow, which, in turn, causes right ventricular dilation and flattening or bowing of the interventricular septum. Pulmonary artery pressure (PAP) increases if thromboemboli occludes greater than 30% to 50% of the total cross-sectional area of the pulmonary arterial bed. In PE, pulmonary vascular resistance (PVR) increases due to the mechanical obstruction of the vascular bed with thrombus and hypoxic vasoconstriction. Local accumulation of inflammatory mediators alters lung surfactant and stimulates respiratory drive resulting in hypocapnia and respiratory alkalosis. PE leads to impaired gas exchange due to obstruction of the pulmonary vascular bed leading to a mismatch in the ventilation to perfusion ratio because alveolar ventilation remains the same, but pulmonary capillary blood flow decreases, effectively leading to dead space ventilation and hypoxemia.Īlso, mediators, such as serotonin, are released, which cause vasospasm and further decreased pulmonary flow in unaffected areas of the lung.  
Pulmonary infarction occurs in about 10% of patients. In contrast, smaller sized emboli block the peripheral arteries and can lead to pulmonary infarction, manifested by intra-alveolar hemorrhage. Large emboli tend to obstruct the main pulmonary artery, causing saddle embolus with deleterious cardiovascular consequences. Pulmonary emboli are typically multiple, with the lower lobes being involved more frequently than the upper, and bilateral lung involvement being more common. Pulmonary embolism occurs when clots break off and embolize into the pulmonary circulation. Hemodynamically stable PE is a spectrum ranging from small, mildly symptomatic or asymptomatic PE (low-risk PE or small PE) to PEs, which cause mild hypotension that stabilizes in response to fluid therapy, or those who present with right ventricle dysfunction (submassive or intermediate-risk PE), but is hemodynamically stable. Patients with hemodynamically unstable PE are more likely to die from obstructive shock (i.e., severe right ventricular failure). Hemodynamically unstable PE (previously called massive or high-risk PE) is PE which results in hypotension (as defined by systolic blood pressure (SBP) less than 90 mmHg or a drop in SBP of 40 mm Hg or more from baseline or hypotension that requires vasopressors or inotropes), the old term "massive" PE does not describe the size of the PE but describes its hemodynamic effect. It is extremely crucial to divide PE based on the presence or absence of hemodynamic stability. 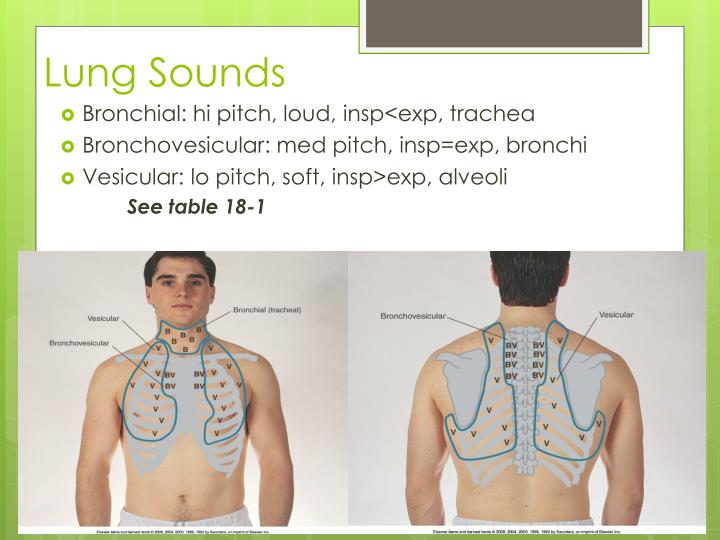
Also, patients with VTE were found to have an increased risk of subsequent stroke and myocardial infarction. Myocardial infarction and congestive heart failure(CHF) increase the risk of PE. Infection anywhere in the body is a common trigger for VTE. Pancreatic cancer, hematological malignancies, lung cancer, gastric cancer, and brain cancer carry the highest risk for VTE. Cancer carries a high risk for thrombus formation and hence, PE.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
